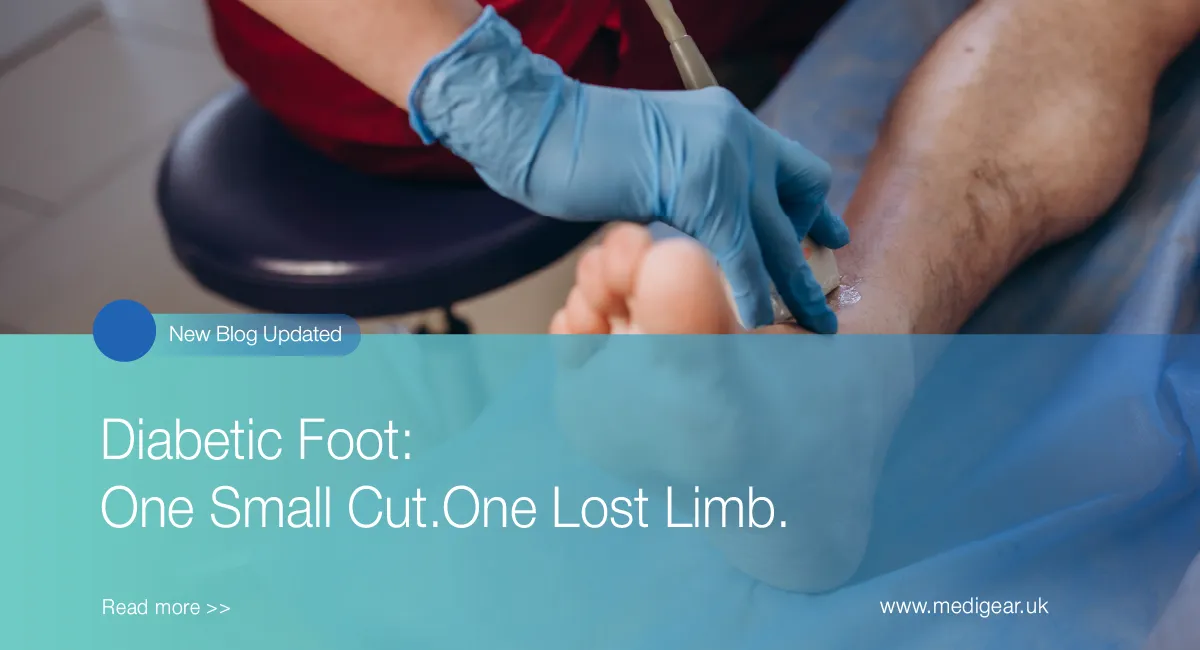
Diabetic foot is not a condition that arrives suddenly. It builds over years — quietly, invisibly — as high blood sugar damages the nerves that carry feeling and the vessels that carry blood to the feet. By the time the damage is bad enough to cause a wound, the patient often cannot feel it. And by the time they can see it, the infection has already taken hold in tissue that heals too slowly to fight back. That is how a papercut becomes a wound, a wound becomes an ulcer, an ulcer becomes an infection, and an infection becomes an amputation that a daily foot check could have prevented.
This guide explains diabetic foot with the honesty this condition demands. How nerve damage sets the trap, how poor blood flow keeps it open, what the warning signs look like, how to prevent the worst outcomes, and how the right clinical equipment supports the foot care that saves limbs. Medigear supplies certified diagnostic and monitoring equipment to hospitals and clinics across the UK — because diabetic foot care is not a luxury add-on. It is the difference between walking and not walking.
Nerve Damage
Nerve damage is the starting point. High sugar over the years wrecks the nerves that carry feeling from the feet to the brain. The damage is slow. It starts with tingling, numbness, or a burn in the toes. Over time, feeling goes completely. A patient with bad neuropathy can step on glass, burn their foot, or get a blister from a tight shoe and feel nothing. The injury happens. The body stays silent. The patient walks on a wound they do not know about — pressing dirt and germs into tissue that is already failing to heal.
Poor Blood Flow
Poor blood flow to the feet makes everything worse. Diabetes harms the vessel walls, narrows arteries, and reduces oxygen delivery to the lower limbs. A healthy foot heals a cut in days. A diabetic foot with poor circulation may take weeks—or not heal at all. Without enough blood, wounds stall. Tissue dies. Infection moves into layers that drugs alone cannot reach. Numb feet plus starved blood supply — that is what makes diabetic foot so deadly and so preventable.
Ulcers
Diabetic foot ulcers are the visible sign that the damage has crossed a line. They usually show up on the sole, toes, or side of the foot — spots that take the most pressure when walking. A callus grows over a pressure point. The tissue under it breaks down. The callus cracks. Under it sits an open wound that the patient never felt forming. Ulcers range from superficial wounds that heal with care to deep, infected holes that extend into bone and require surgery. Depth, blood supply, and infection decide whether the foot can be saved.
Infection
Infection in a diabetic foot moves fast and hides well. The immune system in poorly controlled diabetes does not fight germs as well as in a healthy immune system. Germs get in through a crack, a blister, or an ulcer — and spread through tissue that is weak, poorly fed, and unable to fight back. Skin infection, abscess, bone infection, and gangrene can all grow from a wound that looks like nothing on the surface. Any redness, warmth, swelling, smell, or oozing from a diabetic foot wound needs urgent clinical review. Waiting to see how limbs are lost.
Charcot Foot
Charcot foot is a less-known but devastating problem. Nerve damage weakens the bones and joints. Normal walking causes breaks and shifts that the patient cannot feel. The foot changes shape — swelling, turning red, and taking on a rocker-bottom shape that makes walking painful and prone to ulcers. Early Charcot looks like an infection and is often misdiagnosed. Missing it leads to lasting damage that no surgery can fully undo.
Prevention
Prevention is where the battle is won or lost. Daily foot checks — looking at both feet for cuts, blisters, colour changes, swelling, cracks, and hard skin — catch problems before they become wounds. If you cannot see your feet, use a mirror or ask someone. Good shoes — fitted, supportive, and free of pressure points — cut the stress that causes diabetic foot ulcers. Nail care by trained staff stops the cuts that patients with diabetic foot neuropathy cannot feel. And blood sugar control — the single biggest factor — slows the nerve damage and vessel disease that start the whole chain.
Linked Guides
For clinics managing diabetic patients alongside broader care, our guide to symptoms of kidney problems covers how kidney disease overlaps with diabetes in ways that multiply diabetic foot risk — because kidney failure changes fluid, pressure, and healing in ways that make every wound harder to treat. Our guide to the causes of sudden weakness explains how nerve and vascular damage in diabetes causes symptoms that cross over with diabetic foot presentation — helping clinicians connect systemic disease to limb-threatening problems.
Footwear
Footwear assessment is a clinical step that too many diabetes services skip. A pair of shoes pressing on a numb toe for eight hours creates a wound the patient cannot feel forming. Moulded shoes with pressure-relieving soles and deep toe boxes cut the risk of diabetic foot ulcers by up to half. The shoe is not fashionable. It is a medical tool that belongs in every diabetic foot care plan.
Vascular Assessment
Doppler scans and ankle pressure tests show which patients have blood flow too weak to heal a wound on its own. Opening or bypassing blocked arteries can bring blood back to a dying diabetic foot and turn an amputation into a saved limb. But the window is small. By the time gangrene shows, the chance of saving the diabetic foot has already shrunk. Early testing catches the block before the tissue gives up.
Foot Teams
Teams that bring together diabetes doctors, vascular surgeons, podiatrists, shoe fitters, wound nurses, and infection experts get the best results for diabetic foot patients. No single doctor can handle the full picture. A wound needing offloading, drugs, vascular review, sugar control, and custom shoes all at once needs a team that talks and acts together. Units without a joined-up diabetic foot team lose more limbs than those with one.
Mental Health
Mental health after diabetic foot amputation carries a weight that care pathways rarely see. Losing a limb changes who a person is — their freedom, movement, work, bonds, and self-worth. Depression hits hard. Suicide risk rises. Patients need mental health support built in from the day the wound shows — not added when they stop turning up.
Education
Education is the cheapest and most effective step in diabetic foot care. A patient who knows they cannot feel their feet, that a small cut can cost a limb, and that daily checks take thirty seconds will guard themselves better than any clinic visit can. Yet many diabetes services still treat foot teaching as a leaflet handed out once and never revisited. Teaching patients to check, choose shoes, control blood sugar, and report changes early is not a nice extra. It is the front line of diabetic foot prevention.
Screening
Diabetic foot screening should happen at least once a year for every person with diabetes — and more often for those with neuropathy, poor flow, or past ulcers. A 10-minute check using a monofilament for nerve testing, a Doppler for blood flow, and a visual assessment of the skin gives clinicians the data to assess risk and plan care. Skipping this check is how high-risk feet slip through and show up months later as emergencies that could have been routine visits.
Smoking
Smoking and diabetic foot are a lethal mix that clinics must face head-on. Smoking narrows vessels further, cuts off oxygen to already-starved tissue, and slows healing to a crawl. A diabetic patient who smokes and has neuropathy is walking toward amputation on two tracks at once. Stopping smoking is not lifestyle advice. It is limb-saving medicine.
Certification
Medigear supplies certified diagnostic equipment — including Doppler systems, vascular assessment tools, wound care devices, and patient monitoring systems — to hospitals, diabetic clinics, and podiatry services across the UK. Whether you are building a diabetic foot pathway, upgrading vascular assessment, or equipping a wound care service, our team matches the right tools to your clinical need. Reach out to our team directly for guidance built around the feet that are still walking — and the limbs that still have time to be saved.
Conclusion
A drawing pin. A tight shoe. A crack in dry skin. That is all it takes. One small injury on a foot that cannot feel it, fed by blood that cannot reach it, fought by an immune system that cannot match it. Diabetic foot does not require emergency treatment. It arrives as a whisper — months or years before the wound that costs the limb. The checks take thirty seconds. The shoes cost less than the surgery. The education costs nothing at all. Medigear stands alongside diabetic clinics with certified diagnostic tools and the honest support that foot care demands. Speak to our team today — because the limb that is saved is always the one someone checked in time.
⚠️ This post is for general information only. We do not sell medications or provide prescriptions — Medigear.uk is a medical equipment supplier only.